Strabismus refers to a condition where both eyes are unable to focus on the same target, resulting in misaligned eye directions.
While one eye looks straight ahead, the other eye may turn inward, outward, upward, or downward, causing the lines of sight to deviate.
Strabismus has a prevalence of about 2–4% in children. If not detected and treated early, it can permanently impact vision development.
In adults, it can newly occur due to trauma, cranial nerve disorders, or thyroid eye disease, leading to significant discomfort in daily life along with diplopia (double vision).
Types of Strabismus
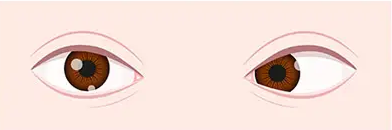
One eye is turned inward (toward the nose).
It is the most common type of pediatric strabismus,
including infantile esotropia and accommodative esotropia.

One eye is turned outward (toward the ear).
Intermittent exotropia is the most common type,
characterized by the eyes drifting outward when tired or in a daze.

One eye is turned upward.

One eye is turned downward.

Causes of Strabismus
Abnormalities in Eye Muscles and Nerves
Misalignment of the eyes can occur due to abnormalities in the six extraocular muscles that control eye movement or the cranial nerves that govern them.
Strabismus may be caused by congenital issues—such as irregular muscle attachment sites or lengths—or by nerve palsy, which weakens specific muscles.
Refractive Error
In cases of severe hyperopia (farsightedness), the eyes must exert excessive accommodative effort to see objects clearly.
This process can cause the eyes to converge inward, leading to a condition known as accommodative esotropia.
Binocular Vision Dysfunction
If the fusional capacity—the brain's ability to merge images from both eyes into a single picture—is weak, eye alignment cannot be maintained,
which may result in strabismus.
Brain and Neurological Disorders
Central nervous system disorders—such as brain tumors, stroke, cerebral palsy, hydrocephalus, and traumatic brain injury—can affect the nerves that control eye movement, thereby inducing strabismus.
Eye Trauma
Strabismus can occur if the extraocular muscles are damaged by trauma around the eye, or if a muscle becomes entrapped due to an orbital fracture (a break in the bones surrounding the eye).
Genetic Factors
If there is a family history of strabismus,
the risk of occurrence increases.

Treatment for Strabismus
Refractive Correction
Refractive errors, such as hyperopia (farsightedness), myopia (nearsightedness), and
콘택트렌즈로 교정합니다.
Strabismus Surgery
Surgery is performed for cases of strabismus that
cannot be corrected with glasses or other non-surgical treatments.
Treatment for Amblyopia
In cases where amblyopia (lazy eye) is accompanied by strabismus,
it is essential to undergo amblyopia treatment concurrently.
Most cases of strabismus do not improve on their own.
오히려 치료하지 않으면 약시가 발생하거나 양안 시기능이 발달하지 못해 영구적인 시력 문제가 생길 수 있습니다.
In pediatric strabismus, if one eye remains constantly misaligned, the brain suppresses the image from that eye, leading to amblyopia—a condition where visual acuity in that eye fails to develop properly.
Amblyopia requires early treatment for vision recovery to be possible, and treatment is most effective when initiated before age 8 to 10. It is crucial to treat both the amblyopia and the strabismus simultaneously.
Accommodative esotropia often resolves with proper alignment of the eyes using corrective glasses alone.
하지만 모든 사시가 안경으로 교정되는 것은 아닙니다. 안경으로 교정되지 않는 사시는 수술이 필요합니다.
Accurate diagnosis is essential to determine the appropriate treatment method.
There is a possibility of intermittent exotropia.
If one eye turns outward when you are tired, spacing out, in pain, or looking into the distance, you may suspect intermittent exotropia.
Check out the blog below for more information on eye health.