"Retinal detachment is a condition where the retina, which lines the inner surface of the eye, becomes separated from its underlying layer (the retinal pigment epithelium).
The retina functions much like the film in a camera, capturing light and transmitting visual information to the brain.
When the retina is detached, its supply of oxygen and nutrients is cut off, leading to damage of the retinal cells.
If left untreated, this condition can result in permanent vision loss.
Types of Retinal Detachment
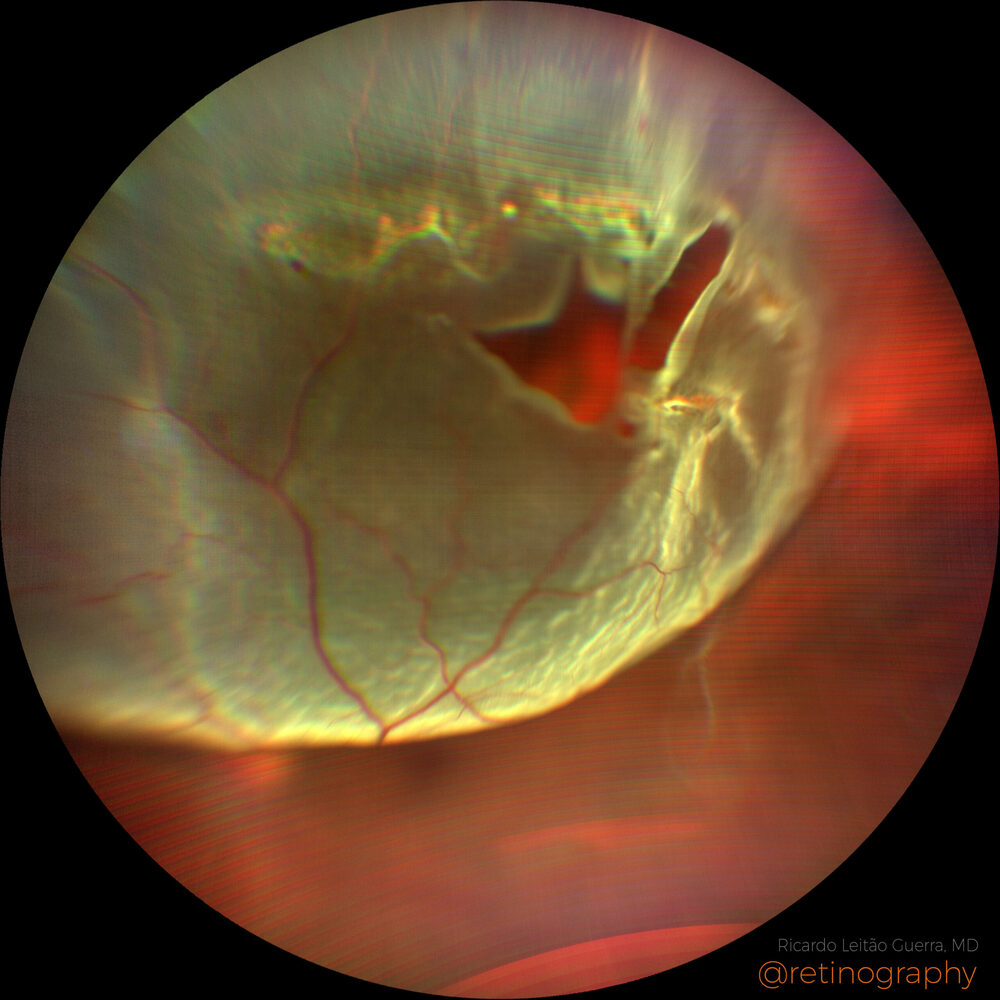
This is the most common type, accounting for approximately 90% of all retinal detachment cases.
It occurs when a hole or tear (break) develops in the retina, allowing vitreous fluid to seep through the gap and lift the retina away from its underlying tissue. The primary causes include age-related vitreous degeneration, high myopia (severe nearsightedness), and physical trauma.
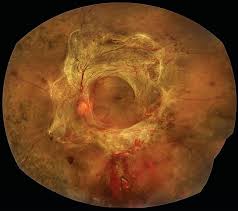
In this type of detachment, fibrous membranes or scar tissue forming on the retinal surface pull the retina away from its underlying layer.
It occurs most frequently as a complication of diabetic retinopathy, retinal vascular occlusion, intraocular inflammation, or post-traumatic complications.
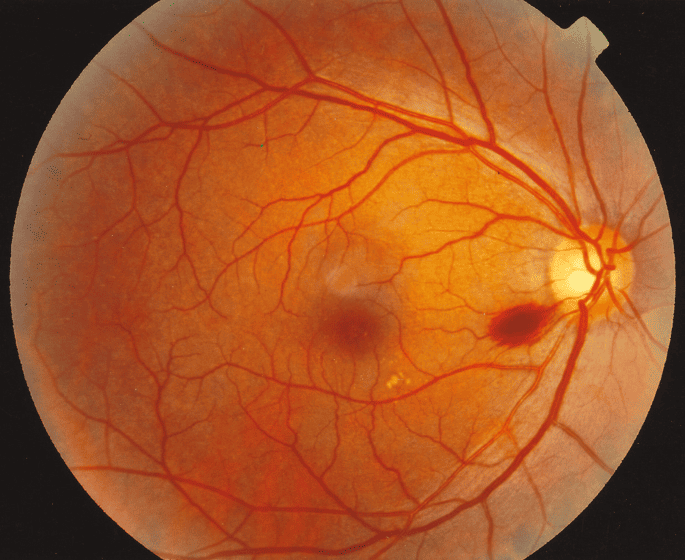
This type occurs when fluid accumulates beneath the retina without the presence of a retinal hole, tear, or traction.
It can be caused by inflammation of the retina or choroid,
intraocular tumors, severe hypertension, or preeclampsia (toxemia of pregnancy).
Symptoms of Retinal Detachment
Retinal detachment may present with few or mild symptoms in its early stages,
but as the condition progresses, the following symptoms may appear:

When retinal detachment occurs, patients may
observe small drifting spots or bright flashes of light within their field of vision.

As a portion of the retina detaches,
patients may experience blurred vision or
the presence of a shadow-like obstruction within their visual field.

Patients may experience visual distortion,
where straight lines appear wavy or objects seem misshapen and distorted.

Patients may experience a sudden onset or a significant increase in floaters,
appearing as drifting spots, threads, or cobweb-like shapes within their field of vision.

Patients may experience a progressive loss of a portion of their visual field in one eye,
or a phenomenon where the vision narrows, similar to tunnel vision.

If the detachment involves the macula, central vision becomes severely impaired,
making it difficult to see objects clearly at the point of fixation.

Retinal Detachment Self-Check
If any of the following apply to you, visit an ophthalmologist.
✔ Floating spots or thread-like objects suddenly increased significantly.
✔ Even with your eyes closed, it looks like light is flashing.
✔ It feels like a black shadow or curtain is falling over the edges of my vision.
✔ Vision suddenly becomes blurry or deteriorates
✔ I recently experienced a strong impact to my eye.

Causes of Retinal Detachment
Posterior Vitreous Detachment
As we age, the vitreous gel that fills the eye shrinks and pulls away from the retina.
During this process, it can tug on the retina, potentially causing holes or tears. The incidence of this condition increases significantly after the age of 50.
High Myopia
Higher degrees of myopia lead to an increased axial length of the eyeball, which causes the retina to become thinner and more susceptible to retinal holes or tears.
Consequently, patients with high myopia are at a significantly higher risk of retinal detachment,
even at a younger age.
Eye Injury
If the eye receives a strong impact from a ball or fist, a traffic
accidents or falls—can cause
significant damage to the retina.
After Cataract Surgery
Following cataract surgery, changes in the vitreous may be accelerated, which can slightly increase the risk of retinal detachment.
Therefore, regular follow-up examinations after the procedure are crucial.
History of Retinal Detachment
If retinal detachment has occurred in one eye,
there is an estimated 10% probability of it developing in the fellow eye. Monitoring both eyes is essential for patients with a prior history.
Diabetes
Diabetic retinopathy can cause
scarring on the retina,
which may lead to retinal detachment.

Retinal Detachment Diagnosis/Examination
Fundus Examination
After dilating the pupils, the entire retina is examined using a special lens.
This is the most fundamental examination that allows direct observation of retinal tears,
the extent of detachment, and the condition of the vitreous.
Fundus Photography
Retinal photographs are taken to document the location and extent of lesions.
Wide-angle fundus photography allows for broad examination
of the peripheral retina.
Ultrasound Examination
When the fundus is difficult to visualize due to vitreous hemorrhage, ultrasound is used to assess the condition of the retina.
It can determine whether the retina is attached or
detached.
Prevention Guidelines for Retinal Detachment

Wear protective eyewear during strenuous exercise or work to prevent eye injuries.
Particular caution is needed if you have high myopia.

We effectively manage systemic diseases such as diabetes and hypertension that affect retinal health.

High-risk groups (those with high myopia, a family history of retinal detachment, a history of cataract surgery, diabetes, etc.)
should undergo regular dilated fundus examinations to detect retinal tears or degeneration early.
Retinal detachment is an ophthalmic emergency. If the macula is still attached, undergoing surgery within 24 to 72 hours is crucial for preserving vision.
Even if the detachment extends to the macula, prompt treatment significantly improves the chances of recovery.
Yes, if retinal detachment occurs in one eye, the risk of it happening in the other eye also increases by about 10%.
Both eyes should undergo regular checkups, and if a hole or degeneration is found in the other eye, consider preventive treatment.
High myopia is a major risk factor for retinal detachment. Get dilated fundus examinations at least once a year, and visit an ophthalmologist immediately if you experience abnormal symptoms such as increased floaters or photopsia. It is advisable to avoid sports involving intense impact.
LASIK, LASEK, and other corneal refractive surgeries themselves do not cause retinal detachment.
However, most people who undergo these surgeries have myopia, and high myopia itself is a risk factor for retinal detachment, so regular check-ups are necessary.