Diabetic Retinopathy is a serious complication that damages the tiny blood vessels in the retina, potentially leading to vision loss.
Chronic high blood sugar weakens these delicate vessels, causing leakage, bleeding, or swelling.
Because early stages often show no symptoms,
the condition can progress silently without you noticing.
Types of Diabetic Retinopathy
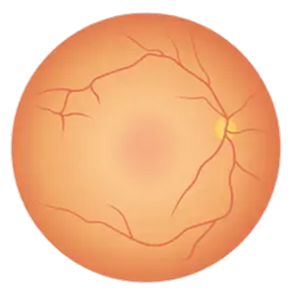
This is the early stage of the disease, where retinal capillaries weaken, leading to microaneurysms, hemorrhages, and exudates.
NPDR is categorized into mild, moderate, and severe stages; the severe stage carries a high risk of progressing to the proliferative phase.
As it is often asymptomatic, regular eye examinations are essential.
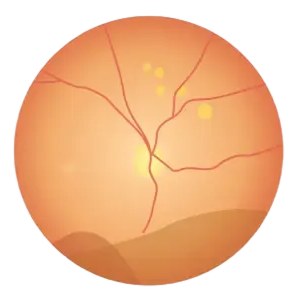
Damaged blood vessels send signals of oxygen deprivation, causing abnormal new blood vessels to grow.
These new blood vessels are extremely fragile and prone to bleeding, which can lead to vitreous hemorrhage or retinal detachment, causing sudden vision loss.
Symptoms of Diabetic Retinopathy
Diabetic retinopathy often lacks early warning signs.
By the time symptoms appear, the condition may have already significantly progressed.
Therefore, regular eye exams are essential for all diabetic patients, even if your vision seems perfectly clear.

You may see spots, threads, or cobweb-like things floating in your vision. This could be an early sign of vitreous hemorrhage.

Your vision fluctuates or appears blurry, as if everything is covered in fog. Vision can change along with blood sugar fluctuations.

It may appear faded, or
color differentiation becomes more difficult than before.

It becomes difficult to distinguish objects in dark environments, and adaptation slows when moving from bright to dark areas.

When macular edema is present, central vision may become blurred, or depending on the location of the hemorrhage, part of the visual field may appear obscured.

If vitreous hemorrhage or retinal detachment occurs,
your vision may suddenly darken partially or completely.
This is an emergency situation, so you must visit the hospital immediately.

Diabetic Retinopathy Self-Check
Diabetic retinopathy is difficult to self-diagnose, so it is important to undergo regular eye examinations.
However, if you experience any of the following symptoms, you must visit an ophthalmologist:
✔️ Floating spots or streaks in your vision
✔️ Blurring or distortion in the center of vision
✔️ Vision deteriorates rapidly
✔️ Vision deteriorates rapidly in dark environments

Causes of Diabetic Retinopathy
Prolonged hyperglycemia
When high blood sugar levels persist,
they damage the walls of the retinal capillaries,
leading to vascular blockages or leakage.
Duration of Diabetes
The longer a person has diabetes, the higher the likelihood of developing retinopathy.
After 15 to 20 years of living with the disease, most patients will show some degree of retinal change.
Poor Blood Pressure Control
High blood pressure puts additional strain on already weakened retinal blood vessels, worsening the damage.
This is why managing your blood pressure is just as critical as controlling your blood sugar.
Dyslipidemia
High cholesterol and triglyceride levels
damage vascular health and promote the accumulation of exudates within the retina.
Kidney Disease
Patients with impaired kidney function or underlying
kidney disease are at a significantly higher risk of developing diabetic retinopathy.
Genetic Factors
If you have poor kidney function or kidney disease,
the risk of developing diabetic retinopathy may increase.

Diagnosis/Examination of Diabetic Retinopathy
After dilating the pupil, the retinal blood vessels and the periphery of the retina are thoroughly examined.
Fundus examination, optical coherence tomography (OCT), retinal angiography, and other detailed examinations

Treatment for Diabetic Retinopathy
Medical Management of Diabetes
Intraocular Antibody Injection
Retinal Laser Treatment
Surgical Treatment
Prevention Guidelines for Diabetic Retinopathy

Because smoking speeds up the destruction of retinal blood vessels, quitting smoking is a must for protecting your eyes.
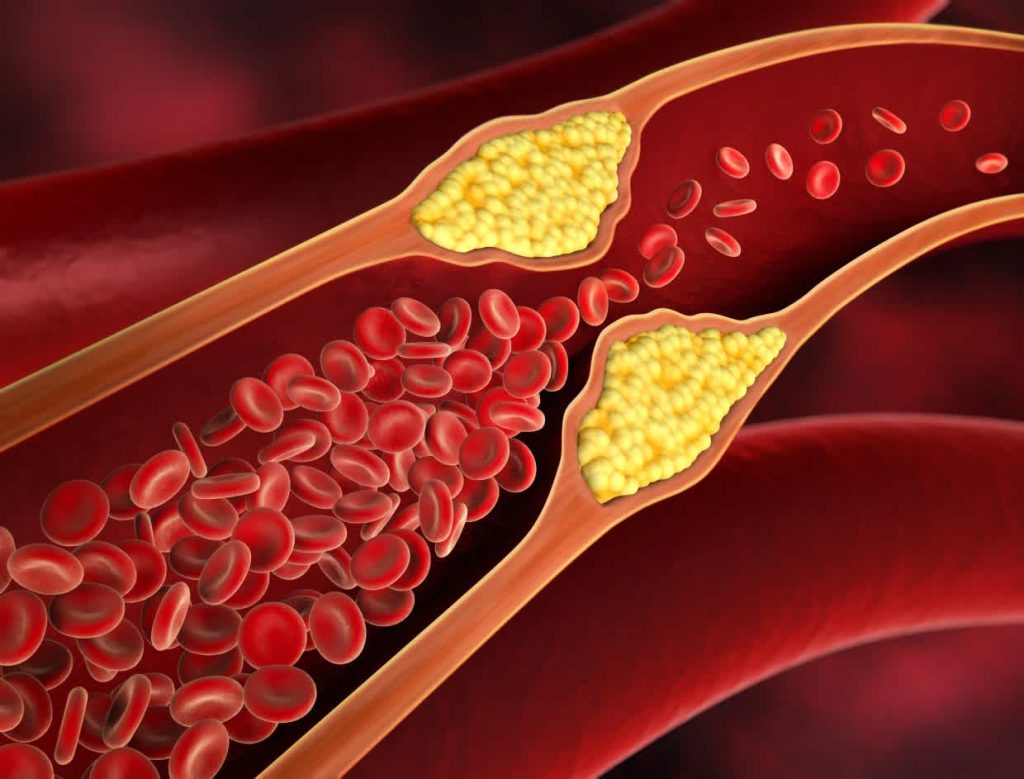
If you have dyslipidemia, actively treat it to maintain vascular health.

Maintain target blood pressure (typically below 130/80 mmHg) to reduce the strain on the retinal blood vessels.

Maintaining your Glycated Hemoglobin (HbA1c) within the target range is the most critical factor.
Proper blood sugar control can significantly delay the onset and progression of retinopathy.
Not all diabetes patients develop retinopathy. However, the risk increases with the duration of the disease.
Proper management of blood sugar, blood pressure, and cholesterol can significantly prevent its onset and progression.
After being diagnosed with diabetes, you should have your first eye exam within five years, followed by regular eye exams thereafter.
If you have had diabetes for a long time, you should have exams more frequently.
To prevent diabetic retinopathy, blood sugar management is most important.
Additionally, regular eye exams and management of conditions such as high blood pressure and high cholesterol are necessary.
It usually affects both eyes, but the degree of progression may differ between them.
If detected in one eye, the other eye should be carefully monitored.